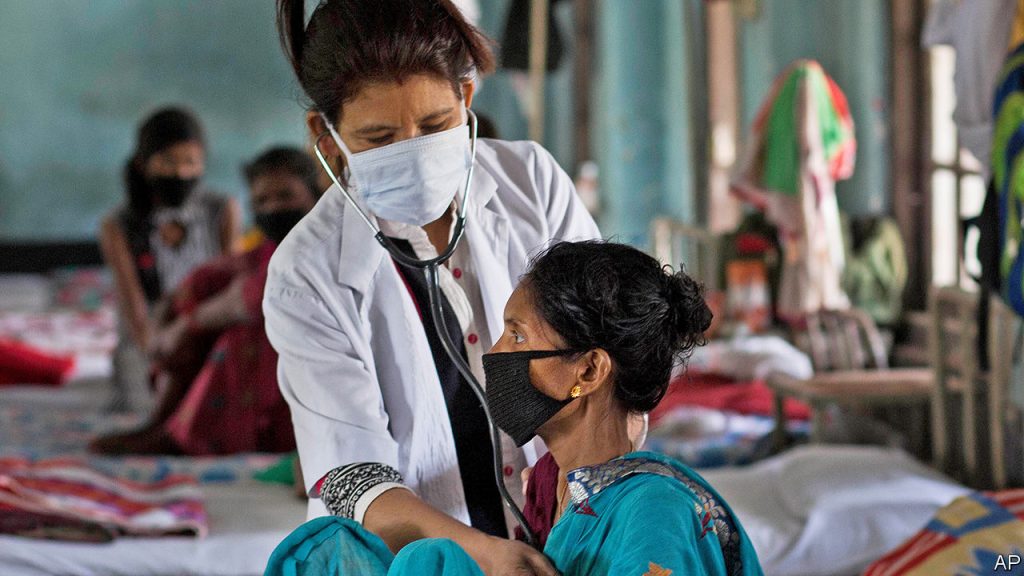
Tuberculosis in South Africa
Tuberculosis (TB) notification rates in South Africa have been declining since 2009, mainly due to increased access to antiretroviral therapy for HIV positive people but also to increases in TB treatment success. However, TB remains the leading cause of death in South Africa which has the highest incidence of TB in the world (834 per 100,000 people). The newly released National Strategic Plan on HIV, STIs and TB proposes two ambitious goals for TB by 2022 (1). Goal 1 is to reduce overall TB incidence by 30%, which can only be achieved by a combination of interventions, for instance by ensuring that everyone infected with HIV is on anti-retroviral therapy, improving the uptake of TB preventive therapy, and successfully identifying and treating the estimated 150 thousand missing TB cases through a national campaign. Goal 2 sets a 90-90-90 target for TB: 1) Find 90% of all TB cases and place them on appropriate treatment, 2) Find at least 90% of the TB cases in key populations and place them on appropriate treatment, and 3) Successfully treat at least 90% of those diagnosed with drug sensitive TB and 75% of those with drug resistant TB. Key populations for TB are, for example: people living with HIV, people living with diabetes, household contacts of people with TB, people working in or living near mines, healthcare workers, and people living or working in prisons.
Current TB case finding strategy
The World Health Organisation recommends systematic symptom screening for active TB in individuals who are seeking health care or who are in health care and belong to selected high risk populations, which include areas where the prevalence in the general population is equal to or higher than 100/100,000 population (2). Although in the South African context this translates to symptom screening of everyone who walks into a public health care facility (so-called “universal” screening) independent of symptomatology, this is not currently part of any policies or guidelines. The South African National Tuberculosis management guidelines of 2009 stated that a “client who presents to a health facility with a cough for more than 2 weeks should be regarded as a tuberculosis suspect and investigated appropriately” (3). The 2014 version of the guidelines states that “every patient with a positive symptom screen must be investigated appropriately” where a positive symptom screen is defined as the presence of any TB related symptom (4) including a cough of more than 2 weeks, fever for more than 2 weeks, current night sweats and recent unexplained weight loss. Among HIV positive people, cough of any duration should be investigated. Investigations following a positive symptom screen currently consist of sputum GeneXpert® (for all presumptive cases) and sputum culture (for HIV positive cases with a negative GeneXpert®). However, symptom screening on its own presents many challenges, especially in a high burden, low resource setting like South Africa.
Diagnostic characteristics of systematic symptom screening
To investigate the effectiveness of screening rules in populations where the general prevalence is higher than 100/100,000 population, we revisited the results from the Zambia South Africa Tuberculosis and HIV/AIDS Reduction (ZAMSTAR) prevalence surveys to assess how well these screening rules perform in identifying TB cases. These communities were selected for the ZAMSTAR trial because of their high burden. In the 2010 survey, around 64,000 people from 8 communities in Cape Town and 16 communities in Zambia provided sputum samples for culture. The average prevalence of TB in the Cape Town communities was 2.4%, and in the Zambian communities 0.6% (5).
Among all participants, without reference to their HIV status, the sensitivity of using coughing for more than two weeks as entry into TB screening was only 20% in the South African group, so that 80% of TB cases would have been missed. The specificity was 95% so that 5 out of 100 TB negative people would be tested unnecessarily for TB. We also investigated the use of combinations of other symptoms in patients who did not have a prolonged cough to increase the sensitivity of screening, while setting a minimum specificity threshold of 85%. One option is to use at least two of the following symptoms: a short duration of cough (< 2 weeks), night sweats or sudden weight loss. This would increase the sensitivity to 35%, allowing an additional 15 out of 100 TB cases to be tested for TB. The specificity using this rule drops to 88% so that 12 out of 100 people would be unnecessarily tested for TB. In other words, in the general population, we would have to use two screening rules in order to increase sensitivity to 35%: (i) prolonged cough and, in those not having a prolonged cough, (ii) at least two of the following symptoms: short cough (<2weeks), night sweats or weight loss.
Exploring other ways to improve TB case finding
Systematic symptom screening in high risk populations, when this translates to screening everyone in the community, is neither sensitive nor cost-effective. To explore alternative methods of improving case finding, we carried out a study in the Buffalo district of the Eastern Cape in 2015 to estimate the proportion of symptomatic TB cases accessing health care that was missed by the health system. The study was designed to represent the population of the district. Adults who visited clinics, for whatever reason, were asked about respiratory symptoms upon exit, and were enrolled in the study if they reported any of the following: coughing, fever, night sweats or recent weight loss. Participants who did not provide sputum samples in the clinics were asked to provide samples to the study staff.
About half of the 1,255 study participants visited the clinics because of their TB symptoms. 80% of them reported that they were screened for TB in the clinic, but only 18% submitted a sputum sample to the clinic staff. Of the traceable results 12% were positive for TB. In the group that visited clinics for reasons other than their current TB symptoms, 20% were screened and 3.7% submitted sputum at the clinic. Of these, none of the traceable results were positive for TB. We managed to obtain approximately 800 evaluable sputum samples from the remaining approximately 1,100 of the participants who did not submit samples in the clinics and identified 39 more TB cases (5%), 3 of which were resistant to rifampicin. Due to the large fraction (50%) of samples submitted in the clinic that had no result recorded in the register, we cannot estimate precisely the fraction of TB cases missed by the health system since these cases might either be truly missed, or cases not recorded in the register but results may have been given to patients and/or patients initiated on treatment (so called “bottom-drawer cases”). Based on simple assumptions we estimate that between 63% and 79% of TB cases were missed among those who attended for their TB symptoms, and between 90% and 100% among those who attended for other reasons. Of the 515 symptomatic participants known to have been in one of the “key populations” (self-reported HIV positive, self-reported diabetes or household contact of TB case), only 48% were screened and only 12% were asked to provide a sputum sample (6).
Using two different approaches to improved case finding, namely (i) improving the sensitivity of symptom screening rules when applied to entire communities and (ii) screening symptomatic primary healthcare clinic attendees on exit, we have shown that symptom screening alone, if used in the community as an active case finding approach (“door-to-door”), would identify at most 35% of TB patients and this is not effective or cost-efficient. A more effective, cost-effective and efficient way would be to screen individuals already accessing healthcare. However, our study in primary healthcare clinics focused on symptomatic individuals only, and recent studies suggest that up to 55% of TB patients might be asymptomatic (7). It is therefore obvious that too many TB patients are asymptomatic for symptom-driven TB screening to be a sufficient case finding tool per se. Screening people who seek health care, for whatever reason, may be a feasible and helpful complementary strategy to symptom-driven testing, and this “universal screening” could have broader criteria for a positive screening test, including other key clinical and demographic characteristics in a screening tool, for instance body mass index, smoking history and previous history of TB.
The TB programme might therefore consider screening all individuals at primary healthcare facility level, irrespective of their reason for attending. The use of a screening tool with improved sensitivity in comparison to symptom screening alone would be preferable, followed by the current diagnostic algorithm. This approach could contribute to reaching the first of the 90-90-90 TB targets as mentioned above, although in what degree would have to be demonstrated by implementation research studies. In addition, it would contribute to Goal 1 of the National Strategic Plan, by identifying some of the missing cases. Ideally a comparison between a campaign, which probably means a “door-to-door” strategy, and universal screening among health care attendees on a national level should be compared to determine feasibility and cost-effectiveness. With the current situation in South Africa, showing only a modest decline in new TB cases since 2012, new avenues and strategies urgently need to be explored, tested and implemented in order to do everything in our power to curb this epidemic and reach the ultimate goal of a South Africa free of TB.